1. Introduction to Intermittent Fasting and Exercise Context
Intermittent fasting (IF) is a dietary pattern characterized by alternating cycles of voluntary fasting and eating within a defined window of time. It is not a specific diet but a schedule for food intake. Common protocols include the 16/8 method (fasting for 16 hours, eating within an 8-hour window), the 5:2 approach (eating normally for five days and significantly restricting calories on two non-consecutive days), and alternate-day fasting. The primary metabolic goal of IF is to extend the period of low insulin levels, prompting the body to shift from using glucose to stored fat as a primary fuel source, a state known as metabolic switching.
When considered in the context of physical performance, a central and complex question arises: can the metabolic adaptations induced by fasting enhance an individual's capacity for exercise? The intersection of IF and exercise performance is a dynamic area of research, with evidence pointing in different directions depending on the type of exercise, the athlete's adaptation period, and their overall nutritional strategy.
- Endurance vs. Strength: Theoretical benefits, such as improved fat oxidation and mitochondrial efficiency, are more relevant to endurance sports. For high-intensity or strength-based activities, the immediate need for glycogen and rapid energy substrates may be compromised during a fasted state.
- Adaptation is Key: The body's response to fasted training is not immediate. It requires a period of adaptation, often several weeks, for physiological systems to adjust efficiently.
- Nuanced Evidence: Current research presents a mixed picture. Some studies suggest potential benefits for body composition and metabolic health, while others indicate a possible negative impact on peak power, strength, and high-intensity endurance, particularly if overall energy and protein intake are not adequately managed.
It is crucial to approach this topic with a balanced perspective, distinguishing between well-established physiological mechanisms and performance outcomes that are still under investigation. The evidence is stronger for IF's role in weight management and metabolic health markers than for its direct, universal performance-enhancing effects.
2. Evidence and Mechanisms: How Intermittent Fasting May Impact Performance
The potential for intermittent fasting (IF) to influence exercise performance is a nuanced topic, with evidence pointing to both potential benefits and significant limitations. The proposed mechanisms are primarily rooted in metabolic adaptations, but their translation to measurable performance gains is highly context-dependent.
The most compelling evidence for a positive impact centers on endurance adaptations. Training in a fasted state (e.g., after an overnight fast) may enhance cellular stress responses. This can stimulate mitochondrial biogenesis and improve the body's efficiency at oxidizing fat for fuel, a process known as metabolic flexibility. For endurance athletes, this could theoretically spare glycogen stores and delay fatigue during prolonged, submaximal exercise.
Conversely, evidence for benefits in high-intensity or strength-based performance is limited and often mixed. Anaerobic activities rely heavily on readily available glycogen. Fasting can deplete these stores, potentially reducing power output, strength, and workout quality. Some studies show no difference or even a decrease in performance metrics like sprint power or muscle protein synthesis rates when training fasted versus fed.
Key mechanisms and the strength of evidence include:
- Enhanced Fat Oxidation (Stronger Evidence): Consistent findings show IF can increase reliance on fat metabolism during exercise, which may benefit ultra-endurance scenarios.
- Autophagy & Cellular Repair (Mechanistic Evidence): Fasting triggers autophagy, a cellular "clean-up" process. While this is well-established in basic science, its direct, measurable impact on human performance recovery is less clear.
- Hormonal Modulation (Mixed Evidence): IF can increase growth hormone and decrease insulin levels. However, the acute performance implications of these shifts are complex and not consistently linked to improved strength or hypertrophy.
It is crucial to highlight the significant limitations in the current research. Many human studies are short-term, involve small sample sizes, or use varied IF protocols (e.g., 16:8 vs. alternate-day fasting), making broad conclusions difficult. Individual factors like training status, sex, diet composition during eating windows, and sleep quality profoundly influence outcomes.
Who should be cautious? Individuals with type 1 or advanced type 2 diabetes, a history of eating disorders, pregnant or breastfeeding women, and those on specific medications should avoid IF without direct medical supervision. Even healthy athletes should consult a sports dietitian or physician to ensure their nutritional strategy supports their performance goals and overall health.
3. Risks, Contraindications, and Who Should Avoid Intermittent Fasting
While intermittent fasting (IF) may offer potential benefits for some individuals, it is not a universally safe or appropriate strategy. A thorough understanding of its risks and contraindications is essential for anyone considering it, particularly in the context of exercise performance.
Established Risks and Adverse Effects
Common side effects, especially during the adaptation phase, can directly impair training quality and daily function. These include:
- Energy Lags and Hypoglycemia: Fasting periods can lead to low blood sugar, causing dizziness, brain fog, and a significant drop in energy, making high-intensity or endurance exercise challenging and potentially unsafe.
- Increased Injury Risk: Training in a fasted or low-energy state may compromise coordination, reaction time, and muscular control.
- Nutrient Deficiencies: A restricted eating window can make it difficult to consume adequate protein, vitamins, and minerals necessary for muscle repair, immune function, and bone health.
- Disordered Eating Patterns: IF can trigger or exacerbate unhealthy relationships with food, obsessive thoughts about eating windows, and binge-eating behaviors.
Clinical Insight: From a sports medicine perspective, the primary concern is mismatching energy availability with energy demand. For athletes or highly active individuals, chronic low energy availability—even if unintentional—can lead to Relative Energy Deficiency in Sport (RED-S), harming metabolism, bone density, and hormonal health. Performance gains are unlikely in this state.
Who Should Avoid or Proceed with Extreme Caution
Strong medical consensus advises against IF for specific populations due to clear risks:
- Individuals with a history of eating disorders.
- Pregnant or breastfeeding women.
- Children and adolescents.
- Individuals with type 1 diabetes or advanced type 2 diabetes, especially those on insulin or sulfonylureas, due to severe hypoglycemia risk.
- Those with significant kidney or liver disease.
Additionally, individuals with the following conditions should only consider IF under direct medical supervision:
- Uncontrolled hypertension or hypotension.
- Active gastrointestinal disorders (e.g., GERD, ulcers).
- Thyroid disorders.
- Those taking medications that require food for absorption or to prevent gastric upset.
Before integrating intermittent fasting into an exercise regimen, a consultation with a physician or a registered dietitian specializing in sports nutrition is strongly recommended. They can help assess individual risk factors, ensure nutritional adequacy, and determine if the potential benefits for performance truly outweigh the risks for your specific health profile and athletic goals.
4. Practical Takeaways for Integrating Intermittent Fasting with Exercise
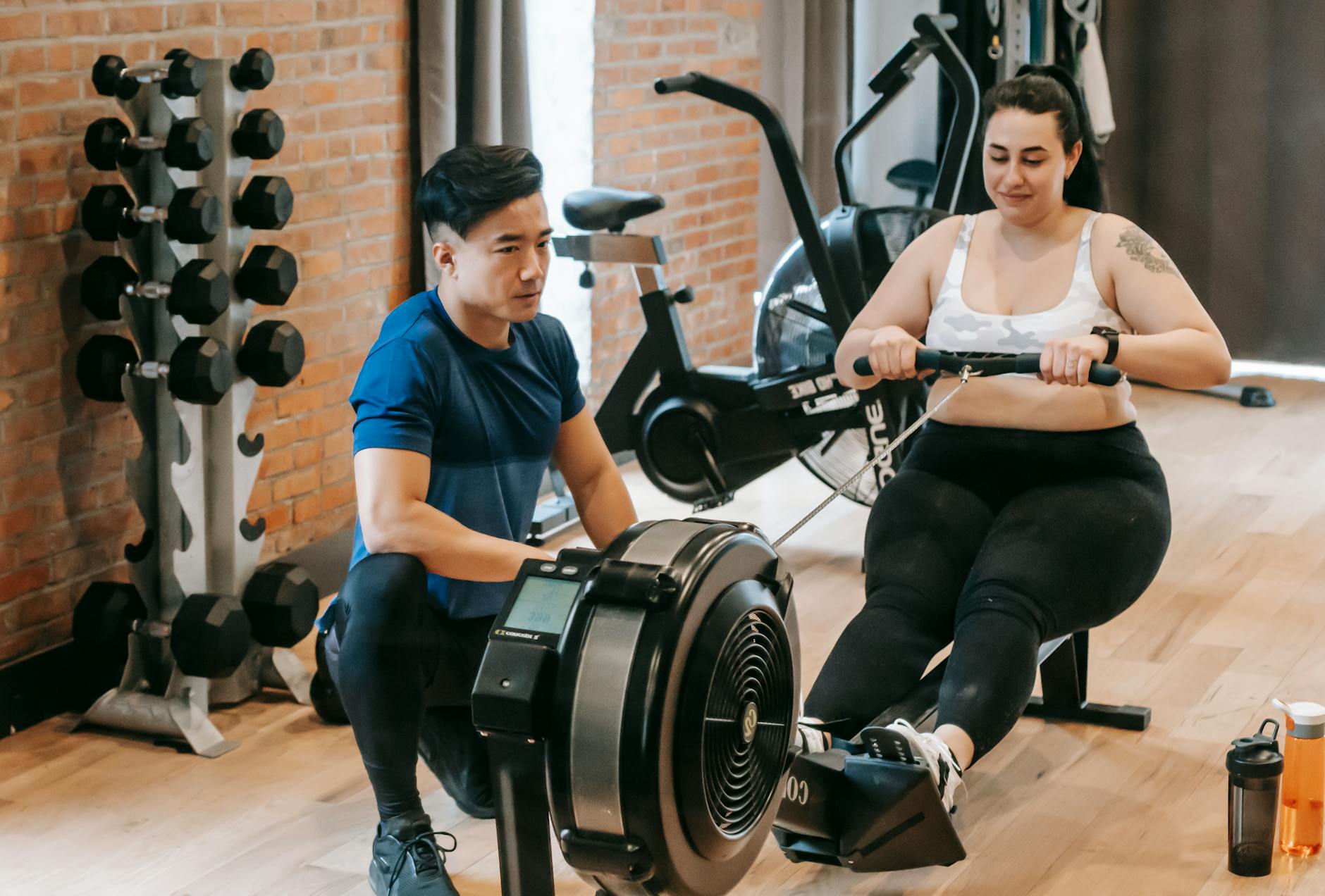
Integrating intermittent fasting (IF) with an exercise regimen requires a strategic and individualized approach to avoid potential pitfalls like energy depletion, poor recovery, or loss of lean mass. The evidence for performance enhancement is preliminary and highly dependent on the type of exercise, the individual's adaptation, and the specific fasting protocol.
A primary consideration is timing. For most individuals, scheduling training sessions during the eating window, or shortly before breaking a fast, is advisable. This ensures fuel availability for higher-intensity workouts like resistance training, sprint intervals, or competitive sports. Low to moderate-intensity steady-state cardio (e.g., brisk walking, light cycling) may be better tolerated in a fasted state and is the focus of most research suggesting enhanced fat oxidation.
- Start Conservatively: Begin with shorter fasting windows (e.g., 12–14 hours) and low-intensity fasted workouts. Monitor energy levels, strength, and recovery closely.
- Prioritize Nutrition: The quality and composition of meals in your eating window are critical. Ensure adequate protein intake (1.6–2.2 g/kg of body weight) to support muscle repair, and consume sufficient carbohydrates around training sessions demanding glycogen.
- Hydrate Relentlessly: Consume water and electrolytes (sodium, potassium, magnesium) throughout the fasting period, especially around exercise, to maintain hydration and neuromuscular function.
- Listen to Your Body: Signs like dizziness, excessive fatigue, a significant drop in performance, or disrupted sleep are indicators that the protocol may need adjustment.
Clinical Insight: The adaptation period to fasted training can take several weeks. During this time, a temporary dip in high-intensity performance is common. The long-term sustainability and benefits are not guaranteed and appear most relevant for endurance athletes seeking metabolic flexibility. For goals centered on maximal strength or hypertrophy, evidence strongly supports training in a fed state with proper peri-workout nutrition.
Who Should Exercise Caution? This approach is not suitable for everyone. Individuals with a history of eating disorders, diabetes (especially Type 1), adrenal dysregulation, pregnant or breastfeeding women, those under significant stress, or athletes in heavy training cycles should avoid integrating IF with exercise without direct supervision from a physician or sports dietitian. The combined metabolic stress can be counterproductive or harmful.
In summary, a practical integration hinges on aligning your fasting schedule with your training demands, emphasizing nutrient-dense refeeding, and maintaining a flexible approach based on physiological feedback. Consulting a healthcare professional before beginning is strongly recommended to assess individual suitability.
5. Safety Considerations and When to Consult a Healthcare Provider
While intermittent fasting (IF) may offer potential performance adaptations for some, it is not a universally safe or appropriate strategy. A clinically responsible approach requires a clear understanding of contraindications, potential risks, and the critical importance of professional medical guidance.
Key Populations Who Should Avoid or Exercise Extreme Caution
Certain individuals should not undertake intermittent fasting without explicit clearance from a qualified healthcare provider. This includes, but is not limited to:
- Individuals with a history of eating disorders: IF can trigger or exacerbate disordered eating patterns.
- Pregnant or breastfeeding individuals: These life stages have significantly increased caloric and nutrient demands that IF protocols may not safely meet.
- People with diabetes (especially Type 1) or hypoglycemia: Fasting alters glucose metabolism and medication requirements, posing a serious risk of dangerous blood sugar fluctuations.
- Those with underlying chronic conditions: This includes kidney or liver disease, adrenal insufficiency, or a history of significant cardiovascular events.
- Children and adolescents: Their bodies require consistent energy and nutrients for growth and development.
- Individuals with low body weight (BMI < 18.5) or nutrient deficiencies.
Common Risks and Adverse Effects
Even for those without clear contraindications, potential adverse effects must be monitored. These can include:
- Excessive hunger, irritability, headaches, and brain fog, particularly during the adaptation phase.
- Increased risk of injury or suboptimal performance if training is attempted in a fasted state with inadequate fueling.
- Potential for overeating or making poor nutritional choices during feeding windows, negating potential benefits.
- Disruption of sleep and hormonal balance in some individuals, particularly with very restrictive protocols.
The evidence for IF's performance benefits is mixed and highly individual; the evidence for these risks in susceptible populations is more consistent and well-established.
Clinical Perspective: From a medical standpoint, IF is an intervention, not a lifestyle default. The decision to use it should follow the same rationale as any other dietary intervention: a clear potential benefit must outweigh the potential risk for that specific individual. It is not a substitute for a balanced, nutrient-dense diet. Athletes should be particularly wary of protocols that may compromise training quality, recovery, or immune function.
When to Consult a Healthcare Provider
You should consult a physician, registered dietitian, or sports medicine specialist before starting IF for exercise performance if:
- You have any of the pre-existing conditions listed above.
- You are taking any medications, especially for diabetes, blood pressure, or mood disorders.
- You experience persistent negative symptoms like dizziness, extreme fatigue, irregular heartbeat, or significant changes in mood.
- Your athletic performance declines, or you face recurrent injuries or illness.
- You have questions about properly timing nutrient intake to support your specific training regimen.
A professional can help you assess personal risk, tailor an approach safely, and monitor biomarkers to ensure the strategy is not causing harm.
6. Questions & Expert Insights
Does intermittent fasting directly increase strength or endurance?
The evidence is mixed and highly dependent on the type of exercise and the fasting protocol. For endurance activities, some studies suggest that training in a fasted state (e.g., morning cardio before eating) may enhance cellular adaptations for fat oxidation, potentially improving metabolic flexibility. However, this does not consistently translate to measurable performance gains like a faster race time. For high-intensity or strength-based training, the data is less supportive. Performing demanding workouts in a fasted state can compromise intensity, volume, and power output due to limited glycogen availability. The potential benefit for performance appears to be indirect, primarily through improvements in body composition (reducing fat mass while preserving muscle), which can enhance power-to-weight ratio in sports like running or cycling.
What are the main risks or side effects, and who should avoid intermittent fasting for exercise?
Common side effects, especially during adaptation, include fatigue, irritability, dizziness, and reduced concentration—all of which can impair workout quality and safety. More serious risks involve nutrient deficiencies, hormonal dysregulation (e.g., disrupted menstrual cycles in women), and the potential loss of lean muscle mass if protein intake and timing are not carefully managed. Intermittent fasting is contraindicated for individuals with a history of eating disorders, pregnant or breastfeeding women, those with type 1 diabetes or advanced type 2 diabetes, individuals with hypoglycemia, and people with certain metabolic or kidney conditions. Adolescents, older adults, and those under significant stress should also approach with extreme caution, if at all.
When should I talk to a doctor before trying intermittent fasting for athletic performance?
Consult a physician or a registered sports dietitian before starting if you have any pre-existing medical condition, take regular medications (especially for diabetes, blood pressure, or mood), are planning for a pregnancy, or have a history of metabolic or hormonal issues. For the conversation, bring a clear outline of your proposed fasting protocol (e.g., 16:8, training timing), your typical training load and goals, and a record of any symptoms you've experienced during past dietary changes. This allows the professional to assess risks related to medication timing, electrolyte balance, and energy availability. They can help you structure a plan that supports, rather than undermines, your health and performance.
Is the timing of my eating window more important than what I eat for performance?
No. Nutritional quality and total energy/nutrient intake remain the most critical factors for exercise performance and recovery. While meal timing can be a useful tactical tool—such as consuming carbohydrates and protein after a strenuous workout to replenish glycogen and stimulate muscle protein synthesis—it cannot compensate for a chronically poor diet. An eating window that leads to inadequate total calorie, protein, or micronutrient intake will ultimately impair performance, adaptation, and immune function. Think of intermittent fasting as a potential framework for meal timing, but the foundation must be built on a balanced, nutrient-dense diet that meets the elevated demands of your training.
7. In-site article recommendations
8. External article recommendations
9. External resources
The links below point to reputable medical and evidence-based resources that can be used for further reading. Always interpret them in the context of your own situation and your clinician’s advice.
-
examine examine.comintermittent fasting – Examine.com (search)
-
wikipedia wikipedia.orgintermittent fasting – Wikipedia (search)
-
mayoclinic mayoclinic.orgintermittent fasting – Mayo Clinic (search)
These external resources are maintained by third-party organisations. Their content does not represent the editorial position of this site and is provided solely to support readers in accessing additional professional information.
