1. Understanding Extreme Cardio: A Clinical Overview
In clinical and exercise science contexts, "extreme cardio" is not a formal diagnosis but a descriptive term for regimens that push cardiovascular and musculoskeletal systems to their chronic limits. It typically involves high-volume, high-intensity aerobic exercise performed frequently, often without adequate recovery. Common examples include daily long-distance running, multi-hour cycling sessions, or high-intensity interval training (HIIT) performed on consecutive days.
The physiological intent of such training is to create a significant adaptive stimulus. However, when the balance between stress and recovery is disrupted, the risk of adverse outcomes increases substantially. It is crucial to distinguish this from the well-established benefits of moderate, regular cardiovascular exercise for heart health, metabolic function, and mental well-being.
Key Physiological Stressors
Extreme cardio imposes a multi-system demand:
- Cardiovascular Strain: Sustained elevated heart rate and cardiac output can, in predisposed individuals, lead to atrial fibrillation, right ventricular dysfunction, or accelerated coronary artery calcification. The evidence for these effects is strongest in lifelong endurance athletes, though causality is complex.
- Musculoskeletal Overload: Repetitive stress without sufficient recovery is a primary cause of overuse injuries like stress fractures, tendinopathies, and chronic joint inflammation.
- Metabolic and Endocrine Impact: Chronic energy deficit, often seen in extreme training, can disrupt hypothalamic-pituitary axes, leading to hormonal imbalances such as low testosterone or estrogen, and thyroid dysfunction.
Clinical Perspective: From a sports medicine viewpoint, the line between peak performance and harm is often defined by individualized recovery capacity. We assess not just workout logs, but sleep quality, nutritional status, psychological stress, and biomarkers of inflammation and hormonal health. The absence of acute injury does not equate to long-term safety.
Evidence and Populations of Concern
Research on the long-term dangers of extreme cardio presents mixed findings, largely due to varying definitions of "extreme" and healthy-participant bias in studies. Strong evidence links it to overuse injuries and relative energy deficiency in sport (RED-S). Evidence for permanent cardiac damage is more limited and often observed in specific genetic predispositions or when combined with other risk factors.
Individuals who should be particularly cautious or seek medical clearance before engaging in such regimens include those with:
- Known or familial cardiovascular conditions.
- A history of stress fractures or significant musculoskeletal injuries.
- Significant nutritional deficiencies or a history of eating disorders.
- Unmanaged autoimmune or inflammatory conditions.
Consulting a sports physician or cardiologist for a pre-participation evaluation is a prudent step for anyone considering a significant escalation in their cardio training volume or intensity.
2. Physiological Mechanisms and Research Findings

Extreme, prolonged cardiovascular exercise imposes significant physiological stress. The primary mechanism involves a sustained elevation in stress hormones, particularly cortisol and catecholamines. While acute elevation is adaptive, chronic elevation from repeated, exhaustive sessions can lead to a state of dysregulation. This hormonal imbalance is a key driver behind several documented adverse effects.
Research findings highlight specific cardiovascular and metabolic consequences. A landmark analysis in the Mayo Clinic Proceedings suggested a U-shaped relationship between exercise dose and long-term cardiovascular health, with the highest volumes of vigorous endurance exercise potentially associated with diminishing returns and increased markers of cardiac stress, such as elevated cardiac troponins and atrial fibrosis. The evidence for this in lifelong elite athletes is more robust than in recreational athletes, but the principle of excessive strain remains.
- Oxidative Stress & Inflammation: Extreme sessions generate high levels of reactive oxygen species (ROS). When antioxidant defenses are overwhelmed, this oxidative stress can damage cells and promote systemic inflammation.
- Immune Function: The "open window" theory posits that intense, long-duration exercise can temporarily suppress immune cell function, increasing susceptibility to upper respiratory tract infections.
- Musculoskeletal Wear: The repetitive load significantly increases the risk of overuse injuries like stress fractures, tendinopathies, and joint cartilage degradation.
It is crucial to distinguish between strong and preliminary evidence. The link between extreme cardio and overuse injuries is well-established. The connection to transient cardiac stress markers is also strong. However, the long-term clinical significance of these markers in otherwise healthy individuals and the direct causal link to serious arrhythmias in recreational athletes remain areas of active research with mixed findings.
Clinical Perspective: From a physiological standpoint, the body requires adequate recovery to adapt positively to training stress. Extreme cardio often violates this principle, pushing systems into a prolonged catabolic state. The risk-benefit ratio shifts negatively when exercise ceases to be moderate-vigorous and becomes chronic, exhaustive exertion without periodization. Individuals with pre-existing cardiovascular conditions, a history of injury, or those new to high-intensity training should be particularly cautious and seek guidance.
Individuals considering or currently engaged in high-volume endurance training should consult a sports medicine physician or cardiologist, especially if they have a personal or family history of heart disease, experience unexplained fatigue, chest pain, or palpitations, or are in a high-risk demographic.
3. Identified Risks and Contraindications

While cardiovascular exercise is foundational to health, extreme cardio workouts—characterized by very high volume, intensity, or frequency—carry specific, well-documented risks. Understanding these contraindications is essential for safe participation.
Primary Physiological Risks
The most robust evidence points to cardiovascular and musculoskeletal overuse injuries. Prolonged, high-intensity endurance training can, in some individuals, lead to transient cardiac stress markers, atrial fibrillation risk, and exercise-induced cardiac remodeling. The musculoskeletal system is also vulnerable, with a high incidence of stress fractures, tendinopathies, and joint degeneration from repetitive impact.
- Overtraining Syndrome (OTS): A complex condition marked by persistent fatigue, performance decline, mood disturbances, and hormonal dysregulation. Diagnosis is clinical, as no single biomarker is definitive.
- Relative Energy Deficiency in Sport (RED-S): A serious syndrome where inadequate caloric intake fails to support physiological function, impairing bone health, immunity, and cardiovascular function.
- Rhabdomyolysis: While rare in structured programs, extreme bouts can cause severe muscle breakdown, releasing myoglobin that risks acute kidney injury.
Populations Requiring Special Caution
Certain individuals should consult a physician—typically a cardiologist or sports medicine specialist—before engaging in extreme cardio. Absolute and relative contraindications include:
- Individuals with known or suspected cardiovascular disease (e.g., cardiomyopathy, coronary artery disease, arrhythmias).
- Those with a history of recurrent stress fractures or diagnosed osteoporosis.
- Individuals with active or recovering eating disorders, due to the high risk of exacerbating RED-S.
- People with uncontrolled metabolic conditions like diabetes or thyroid disorders.
- Anyone experiencing unexplained chest pain, shortness of breath, or dizziness during exercise.
Clinical Perspective: The line between extreme and beneficial cardio is highly individual. A key risk factor is a rapid, unsupervised escalation in training load. We advise thorough pre-participation screening for those with risk factors and emphasize that more is not always better—periodization and recovery are non-negotiable components of a sustainable regimen.
The evidence for these risks is strongest in cohorts of competitive endurance athletes. For recreational athletes, risk is dose-dependent. A balanced approach, incorporating strength training and rest, is critical to mitigating these identified dangers.
4. Balanced Recommendations for Safe Cardio
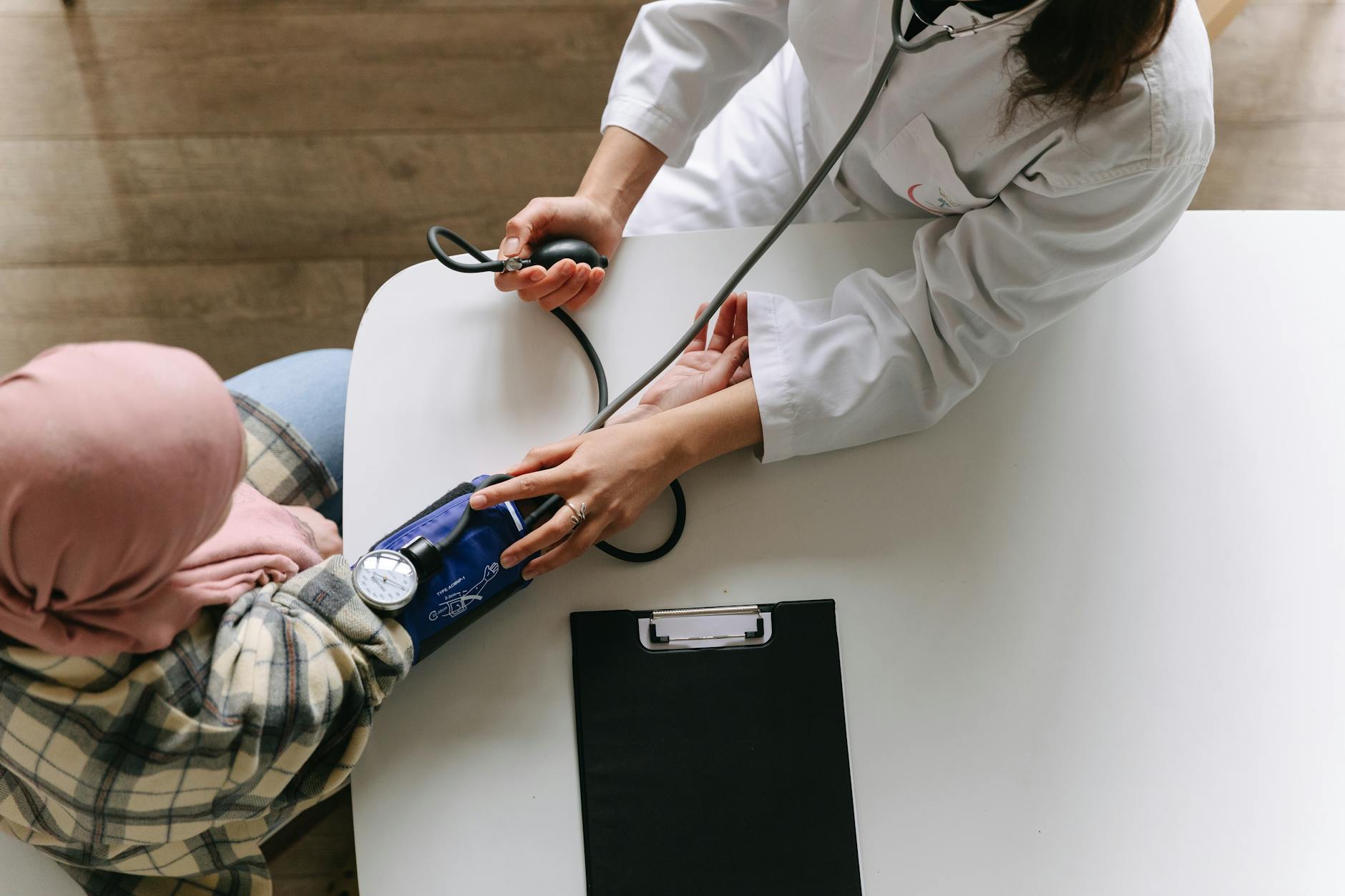
The goal of a sustainable cardio regimen is to harness the well-documented benefits of aerobic exercise—such as improved cardiovascular health, mood regulation, and metabolic function—while mitigating the risks of overuse injuries, hormonal dysregulation, and systemic fatigue associated with extreme volumes. The evidence strongly supports a balanced, periodized approach.
Evidence-Based Guidelines for Volume and Intensity
Major health organizations, including the American Heart Association and the American College of Sports Medicine, provide clear, evidence-based recommendations. For most adults, the consensus is:
- 150 minutes of moderate-intensity aerobic activity or 75 minutes of vigorous-intensity activity per week.
- Activity should be spread across the week, not condensed into one or two extreme sessions.
- Incorporate strength training at least two days per week to support musculoskeletal health and metabolic rate.
These guidelines are derived from large-scale epidemiological studies showing a clear dose-response relationship for health benefits up to these thresholds, with diminishing returns and increased risk of adverse events at significantly higher volumes.
Implementing a Periodized Approach
A key strategy for safety is periodization—systematically varying training load. This is a standard practice in sports science to optimize adaptation and prevent overtraining. A practical weekly model might include:
- Low-Intensity Steady State (LISS): 2-3 sessions (e.g., brisk walking, gentle cycling).
- Moderate-Intensity: 1-2 sessions (e.g., jogging, swimming laps).
- High-Intensity Interval Training (HIIT): No more than 1-2 short sessions (e.g., 20-30 minutes).
- Rest or Active Recovery: At least 1-2 full days dedicated to rest or very light activity like stretching.
Clinical Insight: The "more is better" mindset is a common pitfall. Clinically, we look for non-functional overreaching, signaled by persistent fatigue, performance decline, sleep disturbance, and mood changes. These are red flags that the cardio load is excessive and counterproductive. Listening to these physiological signals is as important as following any numerical guideline.
Essential Components of a Safe Routine
Beyond weekly volume, safety is underpinned by consistent practices:
- Progressive Overload: Increase duration or intensity by no more than 10% per week to allow tissues to adapt.
- Cross-Training: Engage in different aerobic activities (e.g., cycling, swimming, elliptical) to distribute stress across different muscle groups and joints.
- Recovery Nutrition & Hydration: Adequate protein, carbohydrates, electrolytes, and fluids are non-negotiable for repair and performance.
- Sleep & Stress Management: Prioritize 7-9 hours of quality sleep; chronic psychological stress compounds physical training stress.
Who Should Exercise Particular Caution?
Individuals with pre-existing conditions should consult a physician or sports cardiologist before initiating or significantly changing a cardio program. This is especially crucial for those with:
- Known or suspected cardiovascular disease (e.g., hypertension, arrhythmia, history of heart attack).
- Musculoskeletal injuries or chronic joint issues (e.g., osteoarthritis).
- Metabolic disorders like diabetes.
- A history of relative energy deficiency in sport (RED-S) or eating disorders.
The most effective cardio plan is one that is consistent, enjoyable, and responsive to your body's feedback, not one that pushes relentlessly toward an extreme.
5. When to Seek Medical Advice
While regular exercise is a cornerstone of health, the line between vigorous training and potentially harmful overexertion can be thin. Recognizing when symptoms signal a need for professional medical evaluation is a critical component of responsible fitness. This guidance is based on established clinical principles for evaluating exercise-related complaints.
You should consult a physician or a sports medicine specialist promptly if you experience any of the following signs or symptoms, especially if they are new, worsening, or persistent:
- Chest Pain, Pressure, or Discomfort: Any exercise-induced chest symptom, particularly if it radiates to the arm, neck, jaw, or back, or is accompanied by shortness of breath, nausea, or dizziness, requires immediate medical attention to rule out cardiac causes.
- Unexplained Shortness of Breath: Breathlessness that is disproportionate to the exercise intensity, occurs at rest, or is accompanied by wheezing or a feeling of suffocation.
- Palpitations or Irregular Heartbeat: A sensation of a racing, pounding, fluttering, or irregular heart rhythm during or after exercise.
- Persistent, Unexplained Fatigue: A state of exhaustion that does not resolve with adequate rest and recovery, potentially indicating overtraining syndrome, hormonal imbalance, or other underlying conditions.
- Significant Weight Loss or Amenorrhea: Unintended weight loss or, for premenopausal individuals, the cessation of menstrual periods for three or more cycles, which can be signs of Relative Energy Deficiency in Sport (RED-S).
- Recurrent or Severe Injury: Pain that does not improve with rest, recurrent muscle or joint injuries, or stress fractures.
Clinical Insight: From a medical perspective, the context matters greatly. Individuals with known pre-existing conditions—such as cardiovascular disease, hypertension, diabetes, kidney disorders, or a history of eating disorders—should have a consultation with their doctor before initiating or intensifying an extreme cardio regimen. Similarly, those taking medications (e.g., for blood pressure or mental health) should discuss potential interactions with intense exercise. The evidence strongly supports that a pre-participation health screening can identify risk factors and prevent adverse events.
The evidence for these warning signs is well-established in sports and cardiovascular medicine. However, it is important to note that research on the long-term effects of chronic extreme endurance exercise is still evolving, with some studies suggesting potential cardiac remodeling. This underscores the value of personalized medical guidance.
A proactive approach to health involves listening to your body and seeking expert advice when signals deviate from normal training responses. Scheduling a check-up to discuss your fitness regimen is a prudent step for anyone engaging in high-volume or high-intensity training.
6. Questions & Expert Insights
Is it true that excessive cardio can damage my heart?
While moderate cardio is cardioprotective, emerging evidence suggests a potential for adverse cardiac remodeling with chronic, high-volume, high-intensity endurance training. This is often termed "athlete's heart," which is typically benign, but in a small subset, it may progress to issues like atrial fibrillation or, very rarely, myocardial fibrosis. The key distinction is excessive—defined as volumes far beyond public health guidelines (e.g., >60 miles of running per week for years) combined with insufficient recovery. For the vast majority of recreational exercisers, this is not a concern. The benefits of regular, moderate cardio for heart health are overwhelmingly supported by evidence, while the risks are primarily associated with extreme, elite-level endurance pursuits.
What are the signs that my cardio routine might be too extreme?
Watch for both physiological and psychological markers that indicate overtraining and insufficient recovery. Key red flags include: a persistent, unexplained decline in performance; chronic fatigue that interferes with daily life; disturbed sleep or changes in mood (increased irritability, anxiety, or loss of motivation); frequent illness or injury; and dysregulation of normal bodily functions like menstrual irregularities in women (exercise-associated amenorrhea) or a significant, unintentional change in weight. These symptoms suggest your body's adaptive capacity is overwhelmed. Ignoring them and continuing to push can lead to more serious health consequences, including hormonal dysfunction, compromised immunity, and overuse injuries.
Who should be most cautious about or avoid high-intensity cardio workouts?
Several groups should seek medical clearance and potentially modify their approach. This includes individuals with: Known or suspected cardiovascular disease (e.g., history of heart attack, arrhythmia, cardiomyopathy); Uncontrolled hypertension; Significant joint problems (e.g., severe osteoarthritis); and Certain metabolic conditions like uncontrolled diabetes. Additionally, those with a history of eating disorders should be cautious, as intense exercise can sometimes perpetuate disordered patterns. Older adults or complete beginners without a base fitness level should progress very gradually. The principle is to match the exercise stress to the individual's current physiological capacity.
When should I talk to a doctor about my cardio regimen, and how should I prepare?
Consult a physician or sports medicine specialist if you experience any of the warning signs mentioned, if you are in a higher-risk category, or if you plan to drastically increase your training volume (e.g., training for a first marathon). Before your appointment, prepare a concise summary: document your typical weekly workout regimen (type, duration, intensity), note any specific symptoms (e.g., chest discomfort, dizziness, persistent joint pain, extreme fatigue) and their timing, and bring a list of your current medications and supplements. Also, be ready to discuss your personal and family medical history. This information allows the doctor to provide personalized, evidence-based guidance on safe training limits and whether any specific cardiac or musculoskeletal screening is warranted.
7. In-site article recommendations
8. External article recommendations
9. External resources
The links below point to reputable medical and evidence-based resources that can be used for further reading. Always interpret them in the context of your own situation and your clinician’s advice.
-
wikipedia wikipedia.orgextreme cardio workouts – Wikipedia (search)
-
healthline healthline.comextreme cardio workouts – Healthline (search)
-
examine examine.comextreme cardio workouts – Examine.com (search)
These external resources are maintained by third-party organisations. Their content does not represent the editorial position of this site and is provided solely to support readers in accessing additional professional information.
