1. Introduction to Peptide Injection Dosing: Critical Context and Common Oversights

The use of injectable peptides for therapeutic and performance-related goals has moved from niche clinical settings into broader public awareness. This shift has created a significant knowledge gap, where critical dosing principles are often overlooked in favor of anecdotal protocols. A foundational understanding of dosing is not merely about volume or frequency; it is the cornerstone of safety, efficacy, and clinical responsibility.
Dosing is a complex variable determined by the interplay of multiple factors. These include the specific peptide's pharmacokinetics, the individual's body composition and metabolic health, the intended therapeutic goal, and potential interactions with other substances. A protocol effective for one individual under medical supervision may be ineffective or hazardous for another.
Common oversights that this article will address in detail include:
- Misinterpreting Micrograms vs. Milligrams: A critical decimal point error with potentially severe consequences.
- Ignoring Reconstitution Math: Incorrectly mixing peptide powder with bacteriostatic water, leading to inaccurate concentrations.
- Overlooking Individual Variables: Applying a "one-size-fits-all" dose without adjusting for weight, age, or underlying health conditions.
- Neglecting Cyclical Use and Receptor Desensitization: Continuous use of certain peptides can diminish their effect and increase side-effect risk.
The evidence base for many peptides varies widely. Some, like certain growth hormone secretagogues, have more substantial human clinical trial data for specific indications. For many others, the evidence is preliminary, derived from animal studies, small human trials, or anecdotal reports. It is crucial to distinguish between uses supported by robust clinical evidence and those that remain experimental.
Clinical Perspective: From a medical standpoint, the most significant risk is the unsupervised application of potent biochemical signals. Peptides are not inert supplements; they are signaling molecules that can influence hormone pathways, immune function, and cellular growth. Dosing errors can lead to adverse effects ranging from mild irritation and fluid retention to more serious disruptions in glucose metabolism or immune response. Individuals with pre-existing conditions such as hormone-sensitive cancers, autoimmune disorders, kidney or liver impairment, or those who are pregnant or breastfeeding, should exercise extreme caution and must consult a physician.
This chapter establishes the critical context that dosing is a precise, individualized science, not a casual recommendation. The following sections will deconstruct these common oversights with a focus on practical, evidence-aware guidance.
2. Evidence and Mechanisms: Pharmacokinetics and Dose-Response Relationships
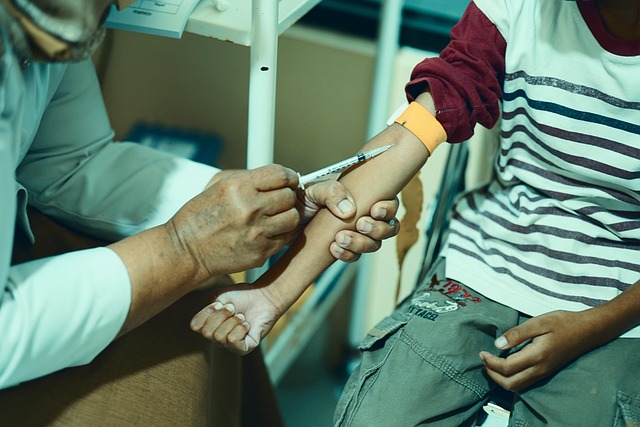
The foundational principle of safe and effective peptide use is understanding its pharmacokinetics (PK)—what the body does to the drug—and the resulting dose-response relationship. This is where many self-administering users make critical oversights, often extrapolating from anecdotal reports rather than clinical data.
For injectable peptides, key PK parameters include:
- Half-life: Dictates dosing frequency. A peptide with a 2-hour half-life requires multiple daily injections to maintain stable levels, while one with a 7-day half-life allows for weekly administration.
- Bioavailability: Nearly 100% for subcutaneous or intramuscular injection, making dose calculations more direct than with oral medications.
- Clearance: How the peptide is eliminated (e.g., renal, hepatic). Impaired clearance organs drastically alter exposure.
The dose-response curve is rarely linear. There is typically a therapeutic window between a minimally effective dose and the point of diminishing returns or increased adverse effects. Exceeding this window does not yield better results and often increases side-effect risk without additional benefit.
Evidence for specific dosing is highly variable. For FDA-approved peptides (e.g., semaglutide, certain growth hormones), PK and dose-response are extensively characterized. For research peptides, data is often limited to animal studies or small, short-term human trials. Dosing protocols from these sources may not translate safely to long-term human use.
Who should be especially cautious? Individuals with kidney or liver impairment must be extremely careful, as altered clearance can lead to dangerous accumulation. Those on multiple medications risk unforeseen interactions. Anyone considering peptide therapy should have these parameters evaluated by a physician and understand that self-dosing based on non-clinical sources carries significant risk.
3. Risks and Contraindications: Adverse Effects and At-Risk Populations
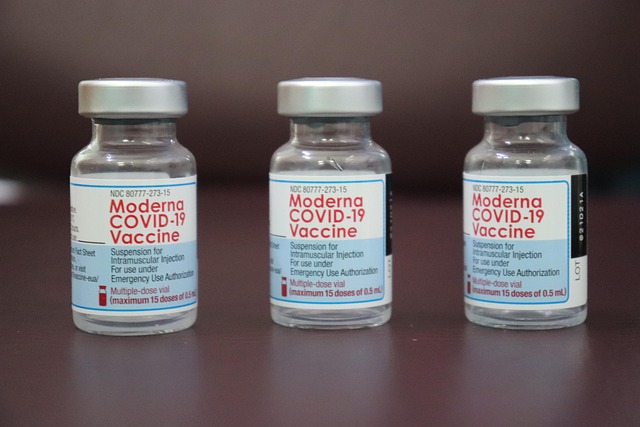
Peptide therapies, while promising, are potent biological agents with a distinct risk profile. A responsible approach requires a clear understanding of potential adverse effects and the populations for whom use is contraindicated or requires extreme caution.
Common and Less Common Adverse Effects
Reported side effects are often injection-site related and mild, including redness, itching, or swelling. Systemic effects can vary significantly by peptide. For example, peptides like GHRPs (Growth Hormone Releasing Peptides) may commonly cause:
- Increased appetite and water retention
- Transient numbness or tingling (paresthesia)
- Joint pain or stiffness
More serious, though less frequently reported, effects can include elevated blood pressure, blood glucose dysregulation, or exacerbation of pre-existing conditions. The evidence for these risks is strongest for peptides with well-characterized mechanisms (e.g., those affecting insulin-like growth factor-1), while data on newer or research peptides is limited and often anecdotal.
Clinical Insight: The dose-dependent nature of side effects is critical. Many users experience no issues at lower "exploratory" doses but encounter significant adverse reactions when escalating without medical supervision. Furthermore, the long-term safety profile for many peptides used off-label for performance or aesthetics remains largely unknown due to a lack of large-scale, longitudinal human studies.
Critical Contraindications and At-Risk Populations
Certain individuals should avoid peptide injections or only proceed under direct specialist supervision. Key contraindications include:
- Active Cancer or History of Certain Cancers: Peptides that influence growth hormone or IGF-1 pathways may theoretically promote tumor growth.
- Pregnancy and Lactation: There is zero safety data for fetal or infant development.
- Severe Kidney or Liver Disease: Impaired clearance can lead to dangerous accumulation.
- Uncontrolled Autoimmune Conditions: Some peptides may modulate immune function unpredictably.
Individuals with the following conditions must exercise extreme caution and consult a physician:
- Diabetes or significant insulin resistance
- Cardiovascular disease, including hypertension
- A history of hormone-sensitive conditions
- Those on complex medication regimens (risk of interactions)
- Individuals with a history of eating disorders, as some peptides affect appetite and body composition.
Ultimately, self-administering peptides without a comprehensive health evaluation overlooks these significant risks. A consultation with a doctor who understands endocrinology and peptide pharmacology is essential to identify individual contraindications and establish a safety monitoring plan.
4. Practical Takeaways: Evidence-Based Dosing Guidelines and Monitoring

Establishing a safe and effective dosing protocol for any peptide requires moving beyond anecdotal reports and anchoring decisions in the available clinical evidence. The most critical principle is that dosing is not one-size-fits-all; it must be individualized based on the specific peptide, its intended use, and patient-specific factors like age, body composition, and concurrent health conditions.
For peptides with FDA approval, such as semaglutide or tirzepatide for weight management, dosing is highly structured. These regimens typically start with a very low "initiation dose" for several weeks to assess tolerability, followed by a predefined "escalation schedule" to a therapeutic maintenance dose. Deviating from this schedule significantly increases the risk of severe gastrointestinal adverse effects.
For research peptides without formal drug approval, evidence is often derived from small, short-term studies. In these cases, extreme caution is warranted.
- Start Low, Go Slow: Initiate at the lowest dose cited in published literature, often for a period of 4-8 weeks, before considering any increase.
- Cycling: Many protocols suggest "cycling" (e.g., 8-12 weeks on, followed by a 4-8 week washout period) to potentially mitigate receptor downregulation and maintain efficacy.
- Source Matters: Dosing accuracy depends entirely on the purity and concentration of the peptide source, which is a major variable with research chemicals.
Essential monitoring is non-negotiable. This should include regular self-checks for injection site reactions and systemic side effects, as well as periodic clinical evaluation. Baseline and follow-up blood work—assessing metabolic panels, liver enzymes, kidney function, and hormone levels—is crucial to objectively assess impact and safety.
Who must exercise extreme caution? Individuals with pre-existing renal or hepatic impairment, those with a history of hormone-sensitive cancers, individuals who are pregnant or breastfeeding, and anyone on complex medication regimens should not initiate peptide therapy without direct supervision from a qualified physician. The interplay with other medications is often unknown.
The most practical takeaway is that an evidence-based approach prioritizes safety and minimal effective dosing over aggressive protocols. It accepts that for many peptides, high-quality long-term human data is limited, making conservative dosing and vigilant monitoring the responsible standard of care.
5. Safety Considerations: When to Consult a Healthcare Professional

While peptides can offer targeted physiological effects, their use is not without risk. A self-directed injection protocol bypasses the critical safety checks of a formal medical evaluation. Consulting a qualified healthcare professional is not merely a suggestion; it is a fundamental component of responsible use. This step is essential for identifying contraindications, establishing a safe baseline, and creating a monitoring plan.
You should schedule a consultation with a physician before initiating any peptide regimen if you have any of the following pre-existing conditions or circumstances:
- Chronic Health Conditions: This includes, but is not limited to, kidney or liver disease, diabetes, cardiovascular conditions, autoimmune disorders, or a history of cancer. Peptides can influence metabolic and immune pathways, potentially exacerbating underlying issues.
- Current Medication Use: If you are on any prescription medications, especially for diabetes (e.g., insulin, GLP-1 agonists), blood thinners, or hormone therapies. The risk of adverse interactions is a significant and often overlooked concern.
- Pregnancy, Breastfeeding, or Plans to Conceive: The safety profile of research peptides in these populations is virtually non-existent. Their use is strongly contraindicated.
- History of Hormone-Sensitive Cancers: Such as breast or prostate cancer. Certain peptides may influence hormonal pathways.
- History of Eating Disorders or Body Dysmorphia: The use of peptides for body composition goals requires careful psychological evaluation to prevent the reinforcement of harmful behaviors.
Clinical Perspective: From a medical standpoint, the consultation serves multiple purposes. First, it allows for a review of systems and relevant bloodwork (e.g., metabolic panel, hormone levels, inflammatory markers) to establish a baseline and rule out silent contraindications. Second, it provides an opportunity to discuss realistic expectations and evidence. Much of the popular data on peptides originates from small studies, anecdotal reports, or preclinical models; a physician can help contextualize this information. Finally, it establishes a relationship for ongoing monitoring, which is crucial for detecting potential adverse effects early.
Furthermore, you should seek immediate medical advice during a cycle if you experience symptoms such as persistent injection site reactions (redness, swelling, pain), signs of systemic infection (fever, chills), severe allergic reactions, unexplained changes in blood glucose, palpitations, or significant mood alterations. Discontinuing use and reporting these symptoms to a doctor is imperative.
Ultimately, the decision to use peptide therapies carries a responsibility for due diligence. Partnering with a knowledgeable healthcare provider is the most effective strategy to mitigate risk and align use with the principles of safety and evidence-based practice.
6. Questions & Expert Insights
How do I know if the dosing information I find online is reliable?
This is a critical question, as much online information is anecdotal, commercially driven, or extrapolated from research not designed for personal use. Reliable dosing guidance is specific to the peptide, its intended purpose, and the individual's health status. Start by looking for sources that cite primary research from peer-reviewed journals, not just forums or vendor websites. Be highly skeptical of "one-size-fits-all" protocols or recommendations that promise rapid, dramatic results. Crucially, dosing for research purposes (e.g., in rodent studies) does not directly translate to human use. The most reliable approach is to have dosing managed by a licensed healthcare provider who understands your full medical history and can interpret the evidence in context. They can tailor a regimen, monitor for side effects, and adjust based on your response, which is impossible with a static online protocol.
What are the most commonly overlooked risks of self-administering peptide injections?
Beyond the obvious risks of infection or improper injection technique, users often overlook systemic and long-term concerns. First is the potential for hormonal and metabolic disruption. Many peptides influence pathways like growth hormone secretion or insulin sensitivity; unmonitored use can lead to imbalances, such as elevated blood glucose or unwanted lipoatrophy. Second is the risk of developing neutralizing antibodies, where the body's immune system reacts to the peptide, potentially rendering it ineffective or causing adverse reactions. Third is the unknown impact on pre-existing conditions, such as stimulating the growth of undiagnosed tumors (a theoretical risk with growth hormone secretagogues) or exacerbating autoimmune disorders. Finally, the purity and sterility of peptides from unregulated sources present a significant, often underappreciated, risk of contamination.
Who should absolutely avoid peptide injections without specialist consultation?
Several populations should consider peptide injections contraindicated or proceed with extreme caution only under direct specialist supervision. This includes individuals with: Active cancer or a history of certain cancers, due to the mitogenic potential of some peptides; Severe kidney or liver disease, as these organs are crucial for metabolizing and clearing peptides; Women who are pregnant, breastfeeding, or trying to conceive, due to a complete lack of safety data; Individuals with a history of eating disorders, as peptides used for body composition could trigger unhealthy behaviors; and Those on complex medication regimens (polypharmacy), due to high risk of unforeseen drug-peptide interactions. If you fall into any of these categories, initiating peptides without a thorough medical evaluation is not advisable.
What should I discuss with my doctor before considering peptides, and what information should I bring?
Initiate this conversation with a focus on safety and evidence. Frame it as a consultation about a potential therapy you are researching. You should bring: 1) Your complete medical history, including all current medications and supplements, 2) Specific, peer-reviewed studies or clinical data on the peptide(s) you're interested in, 3) Your clear, measurable health goals (e.g., "improve recovery from tendonitis" vs. "get ripped"), and 4) Information on the proposed source, if known. Key questions to ask your doctor include: "What are the specific risks for someone with my health profile?" "What baseline tests should we run to ensure safety?" "How will we objectively monitor efficacy and side effects?" and "What are the evidence-based alternatives to achieve my goal?" This prepares your physician to give a nuanced, personalized risk-benefit analysis.
7. In-site article recommendations
8. External article recommendations
9. External resources
The links below point to reputable medical and evidence-based resources that can be used for further reading. Always interpret them in the context of your own situation and your clinician’s advice.
-
healthline healthline.compeptide injection dosing – Healthline (search)
-
mayoclinic mayoclinic.orgpeptide injection dosing – Mayo Clinic (search)
-
examine examine.compeptide injection dosing – Examine.com (search)
These external resources are maintained by third-party organisations. Their content does not represent the editorial position of this site and is provided solely to support readers in accessing additional professional information.
